Small changes in your mouth—like loose teeth, sore gums, or a shifting bite—can be early clues that you need an implant consultation. Acting early keeps your smile healthy and your bite stable.
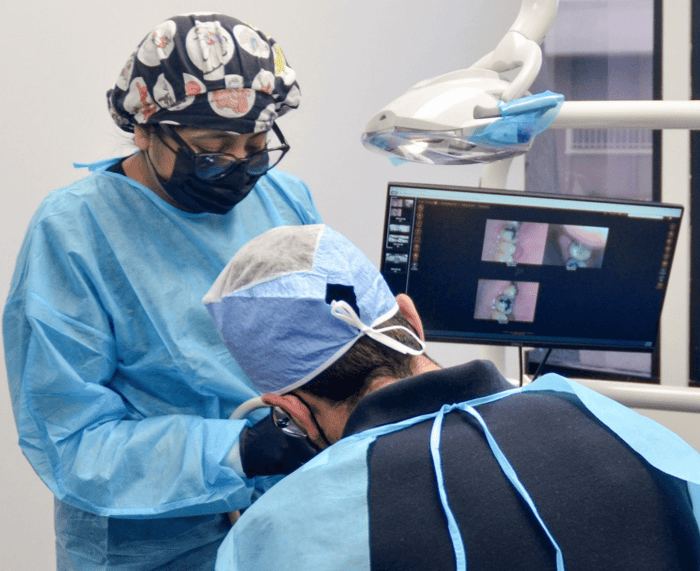
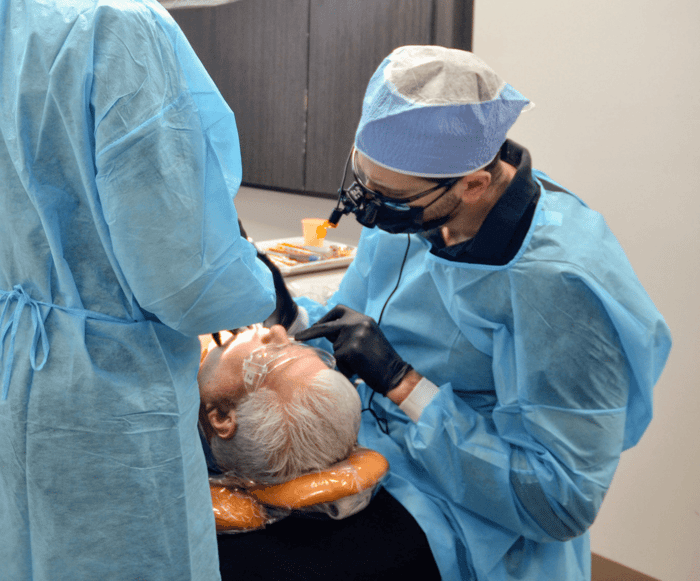
At Gardena Dental Care, our implant specialists evaluate tooth movement, bone health, and gum stability using advanced 3D imaging. We identify problems early and recommend targeted implant options that prevent future bone loss and restore natural comfort.
This article explains the early warning signs, how they affect your oral health, and what to expect when you schedule your first implant consultation.
Key Takeaways
Watch for subtle mouth changes and ongoing discomfort as signals to seek help.
Early checks can prevent bone loss and more invasive treatment later.
An implant consultation clarifies options and next steps.
Recognizing Early Signs You May Need an Implant Consultation
If you notice gaps, changes in bite, or trouble eating and speaking, act sooner rather than later. These signs can affect your jawbone, speech, and the health of nearby teeth.
Missing or Shifting Teeth
A single missing tooth lets nearby teeth drift into the gap. This shifting changes your bite and makes chewing uneven. Over time, moving teeth creates spaces that trap food and make flossing harder. Missing teeth also reduces stimulation to the jawbone.
Without a root, the bone slowly shrinks, which can change your facial shape and make future implant placement harder. If you see a gap, feel teeth moving, or your bite feels different, schedule a consultation to explore replacing missing teeth before more damage occurs.
Difficulty Chewing or Speaking
If you cut food into small pieces or avoid certain foods, your chewing ability may be compromised. Imbalanced chewing puts extra wear on the remaining teeth and can cause pain or fractures.
Speech changes, like new lisps or slurred words, sometimes happen after tooth loss. Teeth help position your tongue and lips for clear speech. If you notice trouble pronouncing sounds, mention it at your implant consultation.
Loose Dentures or Ill-Fitting Bridges
If your dentures slip, click, or cause sore spots, they are not fitting well. Constant adhesive use and readjustments mean the prosthesis no longer suits your mouth. Loose dentures reduce your bite strength and make eating uncomfortable.
Ill-fitting bridges can stress supporting teeth and hide decay underneath. If a bridge rocks or your gums hurt around it, infection or bone loss may be present. Implant-supported crowns or dentures can secure replacements and protect oral health.
Tell your implant specialist about any looseness, discomfort, or changes in fit so they can recommend the right tooth replacement option.
Oral Health Symptoms Signaling Dental Implants May Be Needed
Watch for ongoing pain, infections, or shrinking gums. These problems can mean a tooth can’t be saved, and an implant consultation may help protect your jaw and chewing ability.
Chronic Tooth Pain or Toothaches
If you feel constant or frequent tooth pain, it may come from nerve damage, a failed root canal, or a cracked tooth that can’t be repaired. Pain that wakes you at night, gets worse with pressure, or lingers after cold or heat is a red flag.
You may also notice swelling or a bad taste in your mouth. Those signs often mean an active infection around the tooth root. The dentist will check X-rays and pulp tests to see if extraction and an implant are the safest long-term option.
An implant replaces the whole tooth root and stops ongoing pain when a tooth cannot be saved. Ask about bone health, because you may need a graft before implant placement if infection has caused bone loss.
Persistent Gum Disease or Recession
Recurring gum disease can loosen teeth and erode the bone that holds them. If you notice gums pulling away, deep pockets, or teeth moving, the risk of tooth loss rises, and implants may become necessary.
Gum recession that exposes large parts of the tooth root often leads to sensitivity and decay. Treating the active infection is the first step, but if the tooth is hopelessly loose or bone is gone, an implant can restore function.
The dentist will measure pocket depths, check bone levels on X-rays, and recommend scaling, surgery, or extraction. If you need an implant, they will plan for any gum or bone grafts to get a stable base.
Severe Tooth Decay or Infection
Large cavities that reach the pulp or repeated infections after fillings or root canals suggest the tooth may not be salvageable. If decay destroys most of the crown or a root fracture is present, extraction is often the best option.
A chronic abscess or draining sinus tract shows ongoing infection that can damage surrounding bone. Removing the tooth, treating the infection, and placing an implant later gives a durable replacement that resists future decay.
Before implants, the clinician will clear infection and evaluate jawbone density. If bone loss exists, they may recommend grafting or delayed implant placement to ensure a stable, long-lasting result.
Jawbone and Facial Changes: When to Seek an Implant Consultation
If you notice loose teeth, a hollowed look in your cheeks, or new jaw pain, act early. These signs often point to bone loss or bite changes that an implant specialist can evaluate.
Bone Loss or Bone Deterioration
When a tooth is missing, the jaw no longer gets stimulation at that spot. Over months to years, the bone can shrink through bone resorption. You may see shorter-looking teeth beside a gap or feel areas that seem thinner when you touch your jaw.
A dentist or implant specialist will check bone volume with X-rays or 3D scans. If bone loss is present, they may recommend bone grafting or other procedures to rebuild the jaw before placing an artificial tooth root (implant). Acting sooner makes grafting easier and improves implant success.
Changes in Facial Structure or Sunken Appearance
Losing bone in the jaw can change how your face looks. Cheeks may appear sunken, lips may thin, and you might notice deeper lines around your mouth.
These changes become more obvious as bone loss continues. Dental implants replace the missing root and help maintain the jaw’s shape.
If you worry about a hollowed face or an older appearance after tooth loss, mention this at your consultation. The specialist can compare images over time and explain how implants might support your facial structure.
How Implants Help Maintain Facial Volume
Facial bone loss changes appearance over time. The Mayo Clinic notes that dental implants prevent jaw shrinkage by transferring bite forces to the bone, keeping cheeks and lips supported. This helps maintain a youthful, balanced facial profile.
Jaw Pain or Bite Changes
New jaw pain, trouble opening wide, or a bite that no longer fits together can signal underlying bone or tooth problems. You might chew only on one side or feel pressure when you bite. These issues can come from shifting teeth after tooth loss or from uneven bone loss.
An implant consultation includes an exam of how your teeth meet and whether the jaw joint shows strain.
Fixing the missing tooth with an implant can restore even bite forces and reduce stress on the jaw. The specialist will also look for infection or gum disease that could be causing pain before recommending implant steps.
Dental Implants as a Solution: What to Know Before Your Appointment
Dental implants can restore chewing, stop nearby teeth from shifting, and preserve jawbone. You’ll learn how implants are built, what happens at a consultation, and how artificial roots and crowns work together.
How Dental Implants Work
A dental implant replaces a missing tooth in three parts: a titanium post, an abutment, and a crown. The titanium post goes into your jawbone and acts like an artificial tooth root. Over weeks to months, the bone bonds to the post, giving strong, long-lasting support.
Once the post is stable, the abutment connects the post to a custom-made crown. The crown matches your bite and tooth color, so it looks and functions like a natural tooth. Implants can support a single tooth, a bridge, or secure a denture for a whole arch.
Expect local anesthesia during surgery and a healing period before the final crown goes on.
Implant Dentistry and the Consultation Process
At your consultation, the dentist reviews your medical history and examines your mouth. They take X-rays or a CT scan to measure bone height and plan implant placement precisely. Tell them about medications, smoking, or gum disease because these affect success.
The dentist will explain options: a single implant, an implant-supported bridge, or full-arch implants.
They’ll outline any preparatory work you might need, such as tooth extraction or bone grafting. You’ll also get a timeline, cost estimate, and aftercare instructions so you know recovery steps and follow-up visits.
Understanding Artificial Tooth Roots and Crowns
The titanium post serves as the artificial tooth root and must fuse with your jawbone. Titanium is strong and biocompatible, which lowers the chance of rejection. Good bone volume matters; if bone is low, the dentist may recommend a graft to create a stable base.
The crown is the visible part that replaces the tooth’s chewing surface and shape. Crowns are made from porcelain, ceramic, or zirconia and are matched to your tooth color. The abutment sits between the post and crown and helps transfer bite forces.
With proper care—brushing, flossing, and regular dental visits—implants can last many years and protect surrounding teeth.
Protect Your Smile Before Problems Progress
Catching early implant warning signs can save you from complex procedures later. Shifting teeth, sore gums, and bite changes often mean it’s time for a specialist’s evaluation.
At Gardena Dental Care, we focus on accurate diagnosis and timely implant planning. Our goal is to stabilize your teeth, protect your jawbone, and help you regain full comfort and confidence.
Reach out to schedule a consultation and take the first step toward restoring strength, balance, and lasting health for your smile.
Frequently Asked Questions
This section answers specific, practical questions about when to seek an implant consult, what the visit includes, treatment options like All-on-6, and paperwork that shows implants are medically needed.
What are the warning signs that a dental implant might be necessary?
Missing teeth or gaps can cause shifting and bone loss. Loose teeth, chronic pain, infections, or cracks suggest tooth loss. Other signs include trouble chewing, slipping dentures, bad breath, and a sunken face. If these impact eating, speech, or confidence, see a specialist.
How can you tell if a dental implant is the right choice for you?
Ensure good health and a sufficient jawbone for implants. The dentist reviews your medical history and imaging to assess bone volume. Conditions like gum disease, smoking, or uncontrolled diabetes can affect success, but many issues can be managed beforehand.
Consider your function and goals: implants offer a long-term solution for restoring chewing and preventing bone loss, often better than removable options.
What to expect during your first dental implant consultation?
Expect medical and dental history questions, a mouth exam, and X-rays or a CBCT scan to evaluate bone and tooth roots. The clinician will explain options tailored to your situation. You will discuss timelines, possible bone grafts, sedation choices, costs, and follow-up visits. Ask about success rates and what recovery will look like for your case.