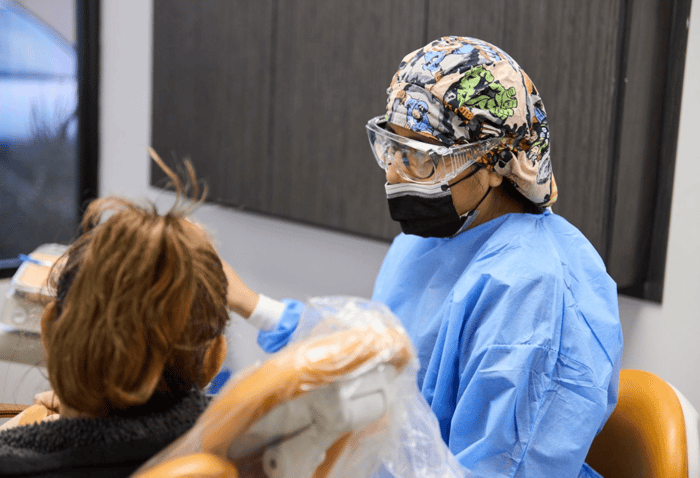
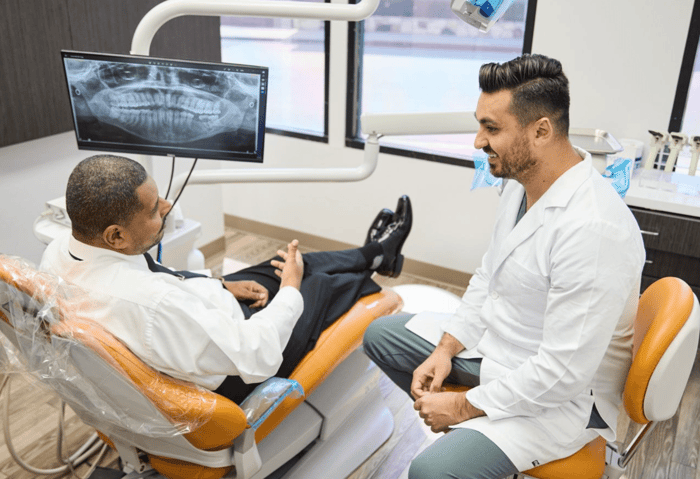
Do you know when facial pressure may signal a dental problem? Facial pressure can come from different sources, but when it’s linked to your teeth or gums, it may point to an underlying issue that needs attention.
At Gardena Dental Care, patients often ask how to determine if facial pressure relates to dental health or other issues like sinus or nerve problems. The key is understanding the patterns, symptoms, and triggers that help identify the source.
In this article, you will learn how dental conditions, sinus problems, and nerve-related issues can all cause facial pressure. You will also discover how to recognize warning signs, when to seek care, and what to expect during diagnosis.
Facial Pressure That Starts with Teeth and Gums
Dental problems often kick off facial pressure in a single tooth or along the gum line. You might feel steady pressure, a pulsing ache, or sensitivity that spreads to your cheek, jaw, or temple.
Key Signs Facial Pressure May Be Dental
Pressure or pain focused around a specific tooth
Swelling in the gums or face near the affected area
Sensitivity to biting, heat, or cold
Bad taste, discharge, or persistent discomfort
Tooth Infection Warning Signs
Tooth infections or dental abscesses usually begin with a sharp or throbbing toothache that gets worse over hours or days. Swelling at the gum near the tooth, a bad taste, discharge, and more pain when you bite are common.
Fever, swollen lymph nodes under the jaw, or puffiness on one side of your face are red flags. Dentists use X-rays and exams to spot abscesses or pulpitis (inflamed nerve tissue). Treatment typically means antibiotics and a root canal or extraction to clear out the infection and ease the pressure.
Why Gum Disease Can Trigger Facial Discomfort
Plaque build-up inflames the gums and kicks off gum disease. Early gingivitis makes gums red and bleed easily; as it advances to periodontitis, infection can eat away at bone and loosen teeth, which creates pressure and aching in the face.
Pockets between teeth and gums trap bacteria, leading to soreness that won’t quit. Dull pressure along the jaw or under the cheek near certain teeth is pretty common. A dental checkup, cleaning, and sometimes gum treatment help cut infection and reduce pressure.
Clues from Cracked Teeth and Fillings
Cracked teeth or failing fillings can let bacteria reach the nerve. You might get sudden pain while chewing, zinging sensitivity to cold, or a constant low ache that spreads into your face.
Cracks often hide, so dentists use X-rays or bite tests to find them. Repairs include bonding, crowns, root canals, or extractions, depending on the damage. Acting quickly usually stops the infection and relieves facial pressure.
Sinus Pressure or Something Else? When Sinuses and Teeth Send Mixed Signals
Sinusitis, dental problems, or both can cause facial pressure. Here’s how to spot the difference and when to seek imaging or a specialist.
Sinus Infections That Masquerade as Tooth Pain
Sinus infections often create pressure above your upper teeth, especially the molars. You might feel a dull ache that worsens when you bend forward, or if you’ve got nasal congestion and thicker drainage.
Yellow or green discharge, fever, and less sense of smell are other clues. ENT providers and dentists both check because maxillary sinus inflammation sits right above those upper back teeth. If symptoms follow a cold and come with nasal blockage, sinusitis is more likely than a tooth abscess.
If pain sticks to one tooth, gets worse with chewing, or the tooth reacts to temperature, a dental cause is more likely. Your provider decides if antibiotics are needed based on the exam and any tests.
Understanding Facial Pressure Patterns
Location gives you hints. Pressure across the forehead, the bridge of the nose, or under the eyes usually means sinusitis. Pressure on one cheek or behind a specific upper tooth points to dental trouble.
Timing helps too. Sinus pressure often changes with posture or time of day. Dental pain is usually steady, sharp, or triggered by biting. Nasal drainage, congestion, or fever go with sinus problems; swollen gums, a visible cavity, or a loose filling suggest dental causes.
When the source isn’t clear, your provider might order dental imaging or a CT sinus scan. These can reveal hidden tooth infections, sinus fluid, or other issues.
How Dental Issues Affect the Sinus Area
Infections in upper back teeth can reach the maxillary sinus because they’re so close together. A tooth abscess might cause facial pressure, sinus inflammation, or even pus draining into your nose. Bad taste, stubborn bad breath, or tooth pain that radiates to your cheek can show up.
Dental x-rays or cone-beam CTs reveal root infections, bone loss, or a sinus floor defect. Treating the tooth—root canal or extraction—usually clears up sinus symptoms if the tooth was to blame. Sometimes, both an ENT and a dentist need to work together if sinusitis and dental infection overlap.
The Role of Nerves and Neurological Causes
Nerve problems can cause facial pressure and pain, not just teeth. Knowing nerve-related signs helps you figure out when to see a dentist or a neurologist.
Understanding How Nerve Pain Affects the Face
Facial pain is not always dental in origin, especially when nerves are involved. The Mayo Clinic notes that conditions like trigeminal neuralgia can cause intense facial pain that mimics dental issues but follows different patterns.
Recognizing nerve-related symptoms helps guide proper diagnosis. This ensures patients receive the right type of care rather than unnecessary dental procedures.
Trigeminal Neuralgia and Nerve-Related Discomfort
Trigeminal neuralgia (TN) hits the trigeminal nerve, which carries facial and mouth sensation. You could feel sudden, sharp, electric shocks on one side, triggered by chewing, talking, or even a light touch. Pain attacks last seconds to minutes, sometimes repeating many times a day.
Atypical trigeminal pain or persistent idiopathic facial pain usually feels like a constant ache, burning, or pressure instead of brief shocks. This kind of pain often ignores regular dental treatments.
Neurologists may use medication, nerve blocks, or other options to calm the nerve. Keeping a pain diary with triggers, location, and duration helps providers tell TN from dental issues.
Distinguishing Nerve Pain from Dental Pain
Dental pain ties to a certain tooth, worsens with pressure, and can show swelling or hot/cold sensitivity. Nerve pain often spreads across the cheek or jaw and isn’t tied to one tooth. It can be sudden and electric or a steady burning pressure that x-rays don’t explain.
If facial pressure sticks around but dental exams and x-rays look normal, ask for a neurological check. Dentists and neurologists may team up. Nerve blocks, MRIs, or more dental exams help sort out whether nerves or teeth are the culprit.
Cluster Headaches and Other Referred Pain
Cluster headaches cause severe, one-sided pain around the eye and temple, sometimes with deep facial pressure.
Attacks come in groups—or “clusters”—over weeks or months. You might see redness in the eye, tearing, or nasal congestion on that side. These headaches are neurologic, not dental. Migraines and other head pain can also send pressure into your jaw, teeth, or cheek.
Referred pain feels like it’s coming from your face, but really starts somewhere else in your head. If facial pressure matches up with your usual headaches, a neurologist can help sort it out. Keep track of timing, symptoms near your eye or nose, and any tooth triggers to guide care.
Jaw Joints, Muscles, and Habits: TMJ and Teeth Grinding
Jaw joint problems, tight jaw muscles, and daily habits can all lead to facial pressure. You might feel pain near your ears, temples, or behind your eyes if the temporomandibular joint or muscles act up. Wisdom teeth pushing on nearby structures can also play a role.
How TMJ Disorders Lead to Facial Pressure
TMJ problems happen when the joint that connects your jaw to your skull gets inflamed, misaligned, or stressed. You might notice aching in front of the ear, dull pressure across the cheek, or clicking when you open and close your mouth.
Muscles around the joint can spasm and feel sore. These tight muscles send pain signals that feel like pressure on your face or temple. Trouble opening wide or a bite that feels “off” adds more strain to the joint and muscles.
If the joint shifts or the cartilage disc slips, pressure can spread to nearby tissues. Watch for jaw stiffness, uneven chewing, or pain that worsens after lots of talking or eating.
Bruxism, Stress, and Jaw Pain
Bruxism means clenching or grinding your teeth—usually at night, but sometimes during the day. Grinding puts stress on the TMJ and facial muscles. Over time, you might get constant pressure or soreness along the jawline, temples, and even behind your eyes.
Stress and anxiety make you more likely to clench your jaw. Look for flattened tooth edges, tooth sensitivity, morning headaches, or a tight jaw when you wake up. Night guards, stress management, and stretching can help relax muscles and ease pressure.
Dentists spot wear patterns and suggest treatments to protect teeth and calm muscles. Addressing bruxism early can prevent ongoing jaw pain and daily pressure sensations.
Impacted Wisdom Teeth: When Pressure Hides Out
Impacted wisdom teeth sit under the gum or press sideways against other molars. You might not see swelling, but the force from an impacted tooth can push on bone and nerves, causing deep, steady facial pressure.
Pain often feels dull and hard to pinpoint—behind the last molar, up into the cheek, or toward the ear. Infection around an impacted tooth can add throbbing and more pressure. You could also notice bad taste, trouble opening wide, or discomfort when chewing on that side.
Dentists use X-rays to confirm impaction and see how a wisdom tooth affects nearby areas. Removing or treating the tooth often gets rid of the hidden pressure and cuts the risk of jaw pain or spreading infection.
When to Seek Help: Evaluation, Diagnosis, and Team-Based Care
Facial pressure that lingers, gets worse, or comes with fever or numbness needs a professional look. Quick, coordinated care can stop small problems from turning into chronic pain.
Getting the Right Diagnosis with Your Dental Team
Start with your general dentist for a focused dental checkup. They’ll look at teeth, gums, your bite, and jaw movement, and ask when the pressure started and what makes it better or worse.
If a tooth infection, impaction, or sinus trouble seems likely, they may order X-rays or send you to a specialist.
Oral surgeons handle surgical issues like impacted wisdom teeth or jaw infections. Prosthodontists or endodontists tackle root canals or complex repairs. Keep a clear list of symptoms, meds, and prior treatments to help speed things up.
Dental Imaging and Modern Evaluation Tools
Dental imaging shows problems you can’t see by looking in your mouth. Your team might use digital x-rays, CBCT (3D dental imaging), or panoramic scans to check roots, bone, and sinuses. These images help spot abscesses, root fractures, and sinus issues.
Imaging is quick and uses low radiation. Dentists explain what each scan means and why it matters. Often, imaging plus a clinical exam gives a clear answer, so you get timely care.
Multi-Specialty Approaches to Chronic Facial Pain
Chronic facial pressure sometimes needs a team. Dentists may work with an ENT if sinus or nasal issues are involved. Neurologists help if nerve pain or odd facial pain is suspected.
Pain management specialists can offer meds, nerve blocks, or targeted therapies if other treatments don’t work. Coordination between providers avoids repeat tests and keeps care focused on relief. Ask them to share records and images so everyone’s on the same page.
Symptoms and Signals You Shouldn’t Ignore
Facial pressure with swelling, ear pain, eye pain, or vision changes can mean infection or other dental trouble. Pay attention to when symptoms start, how they shift, and any nearby signs like fever or bad taste in your mouth.
Facial Swelling and Red Flags
Firm, growing, or painful facial swelling usually signals an infection near a tooth or the gums. If just one cheek, jaw, or under-eye area looks puffy and feels warm, you shouldn't wait around. Swelling that suddenly makes it tough to breathe, swallow, or speak? That's an emergency—no question.
Keep an eye out for these warning signs:
Swelling that gets worse over hours or days
Severe toothache or a constant, dull pressure around a tooth
Tender, red gum areas or a visible bump inside your mouth
Fever or just feeling lousy overall
If swelling pops up after a tooth extraction, root canal, or injury, reach out for help right away. Quick treatment can keep an infection from spreading into facial spaces or deeper tissues.
When Ear, Eye, or Vision Changes Matter
Sometimes, tooth pain or jaw pressure triggers ear pain. A dental abscess or impacted wisdom tooth might be the reason. You could feel a full or popping sensation in your ear, too. If new ear pain shows up with oral symptoms, tell your provider about both.
Eye pain, redness, or vision changes aren’t as common, but they’re serious when paired with facial pressure.
Maybe you notice blurry sight, double vision, a drooping eyelid, or worsening eye pain. That could mean infection spreading toward your sinuses or eye socket. Any vision change? Don’t wait—get urgent medical or dental help.
When tooth pain, facial pressure, ear pain, and vision changes show up together, take it seriously. Share every symptom clearly when you call. That way, you’ll get the right care quickly.
Understand the Source Behind Facial Pressure
Facial pressure can come from dental, sinus, or nerve-related causes, but recognizing the signs helps guide the right response. Paying attention to symptoms like localized pain, swelling, or changes in your bite can help identify when dental care is needed.
At Gardena Dental Care, patients receive careful evaluations to determine the exact cause of facial pressure. This ensures that treatment is accurate, effective, and focused on long-term relief.
If you experience ongoing or worsening facial pressure, do not ignore it. Seeking professional care early can prevent complications and help restore comfort and function.
Frequently Asked Questions
Can Facial Pressure Be Caused by a Tooth Problem?
Facial pressure can be caused by a tooth problem when infection or damage affects the surrounding tissues. This often includes symptoms like localized pain, swelling, or sensitivity to pressure. Identifying these signs early helps ensure timely treatment and relief.
How Do I Know If Facial Pressure Is Sinus or Dental?
You can tell if facial pressure is sinus or dental by looking at patterns and triggers. Dental pain is usually focused on one tooth and worsens with biting, while sinus pressure spreads across the face and changes with position. Additional symptoms like congestion or swelling also help distinguish the cause.
When Should I See a Dentist for Facial Pressure?
You should see a dentist for facial pressure if it is persistent, worsening, or linked to tooth pain or swelling. Early evaluation helps identify the cause and prevent complications. Prompt care can lead to faster relief and better outcomes.
Can Nerve Pain Feel Like Tooth Pain?
Nerve pain can feel like tooth pain because it may radiate across the face and mimic dental discomfort. However, it often lacks clear dental triggers and may not show up on dental exams. A proper diagnosis helps determine the correct treatment approach.